The eighth stage is the second step of stimulating regeneration and synthesis. Increased capillary perfusion and local congestion (due to increased peripheral resistance and prolonged vasospasm time) accelerate blood flow and bring more oxygen to the wound. Nuclear cells and proteins can also promote the conversion of sweat into intercellular fluid. The supplement of oxygen and histamine activates macrophages to swallow damaged cells around the wound and release a large amount of amorphous material that can increase swelling.
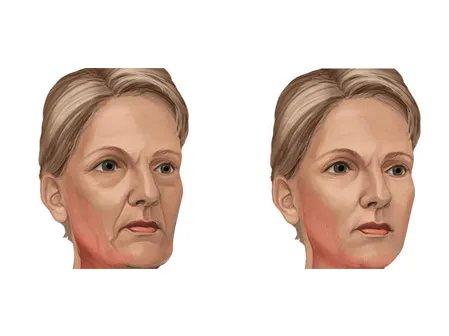
In the ninth stage, the swelling is about to be reduced after 2 to 3 days after the gradual recovery of lymphatic circulation and blood circulation. In the meantime, infrared radiation is used to increase the circulation of tissue lymph fluid.
In the 10th stage, excess oxygen is depleted and the temperature of adjacent tissues rises, which promotes the production of fibroblasts and reduces the activity of macrophages. Peripheral capillaries stimulate stem cells to differentiate into fibroblasts and other cells. At the same time, a large number of cells gather around the PDO thread and form granulation tissue.
In the 11th stage, the fibrinolysis system is activated, and the thrombus in the capillaries gradually dissolves and the blood vessel wall heals. As trypsin, lysokinase, urokinase and plasminogen are released one after another, a new blood exchange network is about to be formed.
In the 12th stage, in this stage, foreign bodies formed by a large number of neutrophils can be seen outside the PDO wire. If there is no further infection, peripheral central granulocytes will rapidly decrease, during which macrophages will migrate and activate, which means wound healing and repair.
The degree of adhesion of macrophages determines the strength of the body's immune response. Even if the adhesion ability decreases a little, the protective function of macrophages will be significantly reduced.
On the other hand, the lysosomes in macrophages can inhibit PDO perilineal fibrosis and the anti-infection ability of centrioles. PDO can significantly reduce the synthesis of macrophage lysozyme and its phagocytic activity, and inhibit its adhesion ability, thereby Prolong the inflammatory response. Some scholars have found that activating the synthesis of antimicrobial peptides helps prevent infection complications after PDO embedding.
In the 13th stage, the immunosuppressive effect can be seen after the PDO thread is partially embedded, and then it is found that both humoral and cellular immunity are weakened. The latter may be related to NK-lymphocytes, but not macrophages.
In the 14th stage, after 3 days, fibroblasts begin to synthesize procollagen and migrate around the wire to form a collagen fiber structure. At first, the collagen fibers are thin, thin, and small in amount. Hyaluronic acid is an amorphous substance located between collagen fibers and prevents lymphocyte adhesion. The synthesis of procollagen is related to vitamin C (ascorbic acid), galactose and glucose, which together form young connective tissue.
The 15th stage is the third step of regeneration and synthesis, namely scar formation and remodeling. With the remodeling of damaged capillaries and granulation tissue, the number of collagen fibers in the extracellular matrix of connective tissue increased significantly.
In the 16th stage, from the 5th to the 7th day, collagen forms collagen fiber bundles. From the second stage, it matures. After a few months, the collagen fiber bundles cross-link to form histidine-hydroxylysine-leucine Three-dimensional structure.
At stage 17, the connective tissue gradually thickens and the number of fibroblasts decreases. The regeneration of connective tissue usually stops on the 21st day after embedding, but the capillaries can still be perfused for 2 to 3 months.
In the 18th stage, the dermis and subcutaneous tissue provide a favorable environment for the formation and growth of collagen and elastin.